The landscape of youth sports has evolved dramatically over the past two decades. While the benefits of physical activity remain undeniable, a concerning trend has emerged in sports medicine clinics across the country. Anterior cruciate ligament (ACL) injuries, once primarily associated with professional or collegiate athletes, are now occurring at alarming rates among youth and adolescent competitors. Recent studies indicate that serious knee injuries, particularly ACL tears, have increased by over 30% in youth sports over the last 15 years. This epidemic of knee injuries not only sidelines young athletes for extended periods but also raises concerns about long-term joint health and the early onset of osteoarthritis.
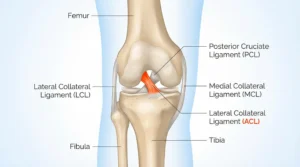
Understanding the mechanics of the knee and the specific vulnerabilities of the ACL is the first step toward reversing this trend. The anterior cruciate ligament is one of the four primary ligaments that stabilize the knee joint, connecting the thigh bone (femur) to the shin bone (tibia). It plays a crucial role in controlling rotational forces and preventing the tibia from sliding too far forward. When an athlete performs high-risk movements such as sudden deceleration, pivoting, or landing awkwardly from a jump, the ACL is placed under immense stress. If this stress exceeds the ligament’s tensile strength, a partial or complete tear occurs. Interestingly, the vast majority of these injuries are non-contact, meaning they happen without a direct blow to the knee.
Several factors contribute to the rising incidence of ACL tears in young athletes. One of the most significant culprits is the shift toward early sport specialization and year-round competition. In previous generations, children naturally cross-trained by participating in different seasonal sports and engaging in unstructured free play. Today, many young athletes focus exclusively on a single sport from an early age, participating in travel leagues and club teams that demand continuous, high-intensity training. This lack of movement diversity prevents the development of well-rounded neuromuscular control and places repetitive stress on the same joints and ligaments. Without adequate periods of rest and recovery, the cumulative fatigue significantly increases the risk of catastrophic injury.
Furthermore, the anatomical and biomechanical differences between male and female athletes play a critical role in injury susceptibility. Research from the Cleveland Clinic consistently shows that adolescent female athletes are two to eight times more likely to suffer an ACL tear compared to their male counterparts in similar sports. This disparity is driven by a combination of factors. Females typically have a wider pelvis, which alters the angle at which the femur meets the tibia (the Q-angle ), potentially placing greater stress on the knee joint. Additionally, female athletes often exhibit different landing mechanics, tending to land with their knees collapsing inward (valgus collapse) and with less knee and hip flexion. This stiff-legged landing posture transfers the impact forces directly to the ligaments rather than allowing the muscles to absorb the shock.
Hormonal fluctuations during the menstrual cycle may also influence ligament laxity, making the ACL more vulnerable at certain times. While anatomical and hormonal factors cannot be changed, biomechanical deficiencies can be addressed through targeted training. This is where proactive injury prevention strategies become essential. The most effective approach to reducing ACL injuries is the implementation of comprehensive neuromuscular training programs. These programs focus on improving biomechanics, enhancing core stability, and teaching proper landing and cutting techniques. By training the nervous system to activate the correct muscles at the right time, athletes can significantly improve their joint stability and reduce the strain on their ligaments.
One of the most widely recognized and successful prevention protocols is the FIFA 11+ program, which was developed specifically to reduce injuries in soccer players but is applicable to many field and court sports. This program incorporates dynamic stretching, plyometrics, core strengthening, and balance exercises. Studies have demonstrated that when teams consistently perform these structured warm-up routines at least twice a week, the incidence of severe knee injuries can be reduced by up to 50%. The key to success is consistency and proper technique. Coaches and trainers must emphasize the quality of movement, ensuring that athletes maintain proper knee alignment and avoid the dangerous inward collapse during dynamic activities.

For athletes looking to optimize their performance and protect their joints, integrating chiropractic care into their routine can be highly beneficial. As detailed in our guide on The Athlete’s Guide to Chiropractic Care Performance Recovery and Injury Prevention, regular adjustments help maintain proper spinal alignment and pelvic balance. When the pelvis is misaligned, it can create compensatory movement patterns that place uneven stress on the lower extremities, including the knees. By ensuring optimal biomechanical function from the core outward, chiropractic care supports the body’s natural ability to move efficiently and safely. Furthermore, soft tissue therapies and targeted exercises prescribed by a chiropractor can address muscle imbalances and improve flexibility, both of which are crucial for injury prevention.
Maintaining proper posture is another often-overlooked aspect of joint health. As discussed in Proper Posture 101 A Complete Guide to Healthy Alignment, the way we hold our bodies during daily activities directly impacts our movement mechanics during sports. Poor posture can lead to tight hip flexors, weak glutes, and altered movement patterns that increase the risk of lower extremity injuries. By addressing postural deficiencies and focusing on core strength, athletes can build a solid foundation that supports dynamic athletic movements. This holistic approach to wellness is essential for long-term athletic success and injury avoidance.
Despite the best prevention efforts, injuries can still occur. If a young athlete experiences a popping sensation in the knee, rapid swelling, or a feeling of instability during activity, immediate medical evaluation is imperative. According to the Johns Hopkins Medicine Sports Injury Statistics, sprains and ligament injuries remain among the most common sports-related conditions, making early diagnosis and intervention critical. Continuing to play on a compromised knee can lead to further damage to the meniscus or articular cartilage. The road to recovery following an ACL tear is long and challenging, typically requiring surgical reconstruction followed by nine to twelve months of intensive rehabilitation. The rehabilitation process focuses on restoring range of motion, rebuilding muscle strength, and gradually reintroducing sport-specific movements.
During the recovery phase, finding natural ways to manage discomfort is important. Our comprehensive resource, The Complete Guide to Natural Relief for Back and Neck Pain, offers valuable insights into managing pain without relying solely on medication. Techniques such as ice therapy, elevation, and gentle mobilization can help reduce inflammation and promote healing. Working closely with a sports medicine professional and a physical therapist ensures that the athlete progresses safely through each phase of recovery, minimizing the risk of re-injury upon returning to sport. The CDC’s HEADS UP program also provides excellent resources for athletes, parents, and coaches navigating the complexities of sports injury recovery.
In conclusion, the rising rate of ACL tears in young athletes is a complex issue driven by early specialization, intense competition schedules, and biomechanical vulnerabilities. However, it is not an inevitable consequence of youth sports. By prioritizing neuromuscular training, encouraging cross-training, and emphasizing proper movement mechanics, we can significantly reduce the risk of these devastating injuries. Parents, coaches, and healthcare providers must work together to create a culture that values long-term athletic development and joint health over immediate competitive success. Through education, proactive prevention strategies, and comprehensive care — including the support of chiropractic and rehabilitation professionals — we can keep our young athletes healthy, active, and performing at their best for years to come. For additional guidance on sports injury rehabilitation, explore our Sports Injury Rehabilitation resources on the blog.